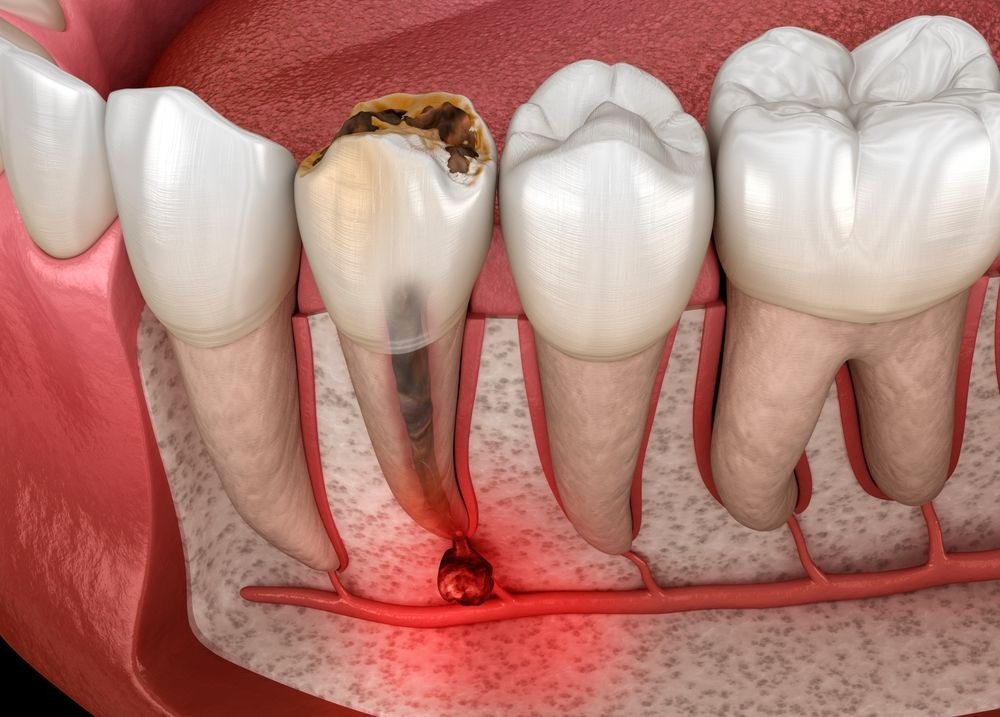
From $3,500 to $500: How One Dental Group is Making Root Canals Accessible to Working Families
Root canal therapy represents one of the most significant financial barriers in preventive dental care. Traditional pricing structures often push necessary treatments beyond the reach of working families, creating a cycle where minor dental issues escalate into complex, expensive problems. When patients delay or avoid root canal procedures due to cost, the resulting complications frequently require more invasive treatments, including tooth extraction and replacement options that can cost substantially more than the original therapy.
The challenge extends beyond individual patient outcomes. Dental practices face operational pressures when a significant portion of their patient base cannot afford recommended treatments. This creates scheduling inefficiencies, reduces case acceptance rates, and often forces practices to refer patients to emergency services where costs are even higher. The current pricing model for endodontic care has created a structural problem that affects both patient health outcomes and practice sustainability.
Recent developments in dental care delivery models suggest that dramatic cost reductions are possible without compromising treatment quality. These changes reflect broader shifts in healthcare economics, where providers are finding ways to maintain clinical standards while addressing affordability concerns that have historically limited access to essential dental services.
Understanding the Cost Structure of Root Canal Therapy
The traditional pricing model for endodontic procedures reflects multiple cost factors that have remained largely unchanged for decades. Equipment costs, specialist training requirements, and insurance reimbursement structures have created a baseline expense structure that typically ranges from $1,500 to $3,500 per procedure, depending on tooth complexity and geographic location. This pricing reflects real operational costs but often places treatment beyond the reach of patients without comprehensive dental insurance.
Alternative approaches to affordable care dental services root canal therapy are emerging through operational efficiency improvements rather than reduced clinical standards. These models focus on streamlined procedures, optimized scheduling systems, and volume-based cost structures that can significantly reduce per-procedure expenses. The key insight driving these changes is that endodontic care can be delivered effectively through standardized protocols that reduce chair time while maintaining clinical outcomes.
Volume-based pricing models allow dental groups to spread fixed costs across larger patient populations. When practices can predict consistent procedure volumes, they can negotiate better rates for materials, optimize staff utilization, and invest in efficiency-enhancing equipment. This approach contrasts with traditional fee-for-service models where each procedure must cover a proportional share of all practice overhead costs.
Operational Efficiency and Clinical Standardization
Standardized treatment protocols represent the foundation of cost-effective endodontic care. Rather than customizing every aspect of treatment delivery, successful affordable care models establish evidence-based procedures that can be delivered consistently across multiple cases. This standardization reduces procedure time, minimizes material waste, and allows support staff to handle routine aspects of patient care more effectively.
Technology integration plays a crucial role in these efficiency gains. Digital imaging, rotary instrumentation, and standardized irrigation systems can reduce treatment time while improving clinical predictability. When these technologies are implemented systematically rather than on a case-by-case basis, the cost per procedure decreases substantially. The initial investment in technology is offset by reduced chair time and improved treatment outcomes.
Staff training and role optimization also contribute to cost reductions. When dental assistants and hygienists are trained to handle specific aspects of endodontic procedures, dentists can focus on the clinical decisions and technical procedures that require their specialized training. This division of responsibilities improves overall productivity without compromising patient care quality.
Insurance and Payment Structure Innovations
Traditional dental insurance often provides limited coverage for endodontic procedures, leaving patients responsible for significant out-of-pocket expenses. Alternative payment structures are addressing this gap through direct-pay models, membership plans, and financing options that spread treatment costs over manageable periods. These approaches remove insurance reimbursement delays and administrative costs from the pricing equation.
Membership-based dental plans offer predictable monthly payments in exchange for covered procedures at predetermined rates. For root canal therapy, this model allows practices to guarantee pricing while patients avoid large upfront payments. The predictable revenue stream helps practices optimize their operations while providing patients with clear, upfront cost expectations.
Direct-pay models eliminate insurance administrative costs and reimbursement uncertainties. When practices can collect payment directly from patients without insurance intermediaries, they can offer reduced rates while maintaining profitability. This approach works particularly well for patients whose insurance provides limited endodontic coverage or who lack dental insurance entirely.
Quality Assurance in Low-Cost Endodontic Care
Maintaining clinical standards while reducing costs requires systematic quality assurance measures that go beyond traditional practice management approaches. Successful affordable care models implement comprehensive outcome tracking, standardized material specifications, and continuing education requirements that ensure cost reductions do not compromise treatment effectiveness. These measures address the legitimate concern that reduced pricing might indicate reduced clinical quality.
Outcome measurement becomes particularly important in high-volume, cost-reduced practice models. Tracking success rates, complication frequencies, and patient satisfaction scores provides objective evidence that affordable care maintains clinical standards. According to the American Dental Association, successful endodontic treatment should result in symptom resolution and radiographic healing in over 85% of cases, regardless of the practice model used to deliver care.
Material standardization helps ensure consistent quality while achieving cost efficiencies. Rather than using premium-priced materials for all cases, evidence-based material selection can identify cost-effective options that provide reliable clinical outcomes. This approach requires careful evaluation of material performance data but can significantly reduce per-procedure costs without affecting success rates.
Provider Training and Certification Requirements
Affordable care models often rely on general dentists rather than endodontic specialists to deliver root canal therapy. This approach can reduce costs substantially, but it requires comprehensive training programs and ongoing competency verification. Successful programs establish clear case selection criteria, ensuring that complex cases are referred to specialists while routine procedures are handled by trained general dentists.
Continuing education requirements become more critical in affordable care settings where volume pressures might encourage shortcuts. Regular training updates, case review sessions, and competency assessments help maintain clinical standards across all providers. These requirements represent an investment in quality assurance that supports both patient outcomes and practice reputation.
Case selection protocols help ensure appropriate treatment recommendations. Not every endodontic case is suitable for streamlined, cost-reduced treatment approaches. Clear criteria for case complexity, patient medical history considerations, and anatomical factors help providers make appropriate treatment recommendations and referrals when necessary.
Equipment and Technology Considerations
Cost-effective endodontic care requires balanced equipment investments that improve efficiency without creating unsustainable overhead costs. Digital radiography, rotary instrumentation, and electronic apex locators represent technologies that can improve treatment outcomes and reduce procedure time, but they require significant upfront investments that must be justified through increased patient volume.
Equipment standardization across multiple locations allows dental groups to achieve better purchasing terms and simplified maintenance contracts. When the same equipment is used consistently, staff training becomes more efficient, and replacement part inventory can be optimized. These operational efficiencies contribute to overall cost reductions that can be passed on to patients.
Maintenance and replacement planning becomes more critical in high-volume practices where equipment failure can significantly impact operations. Preventive maintenance schedules, backup equipment availability, and rapid repair procedures help ensure consistent service delivery while managing long-term equipment costs.
Patient Selection and Treatment Planning
Effective affordable care programs require careful patient selection and treatment planning that balances cost considerations with clinical appropriateness. Not every patient or clinical situation is suitable for streamlined, cost-reduced endodontic care. Successful programs establish clear criteria for patient eligibility, case complexity assessment, and treatment modification options that ensure appropriate care delivery.
Medical history evaluation becomes particularly important when cost constraints might limit treatment options. Patients with compromised immune systems, bleeding disorders, or other medical complications may require modified treatment approaches that affect both clinical procedures and associated costs. Clear protocols for medical history assessment help ensure appropriate treatment recommendations.
Tooth assessment criteria help determine which cases are suitable for standardized treatment approaches. Factors such as root canal anatomy, previous restorative work, and periodontal condition all influence treatment complexity and success probability. Systematic evaluation criteria help providers make consistent decisions about treatment appropriateness and cost estimates.
Treatment Modification Options
Flexible treatment planning allows providers to modify procedures based on individual patient needs while maintaining cost-effectiveness. Options might include staged treatment delivery, alternative restoration approaches, or modified follow-up schedules that accommodate both clinical requirements and patient financial constraints. These modifications require clear protocols to ensure clinical standards are maintained.
Alternative restoration options can significantly affect total treatment costs. While root canal therapy addresses the endodontic problem, the final restoration choice affects both immediate costs and long-term success rates. Cost-effective programs often include comprehensive treatment planning that considers both endodontic and restorative costs in initial treatment recommendations.
Follow-up scheduling optimization helps balance clinical monitoring requirements with cost considerations. While regular follow-up appointments are essential for monitoring treatment success, scheduling efficiency and telemedicine options can reduce the total cost of care while maintaining appropriate clinical oversight.
Practice Management and Operational Efficiency
Successful affordable care delivery requires comprehensive practice management systems that optimize scheduling, reduce administrative overhead, and streamline patient flow. These operational improvements often provide the margin that allows significant cost reductions while maintaining profitability. The focus shifts from maximizing revenue per procedure to maximizing efficiency across the entire patient experience.
Scheduling optimization becomes critical when volume increases are necessary to support reduced pricing. Block scheduling for similar procedures, standardized appointment lengths, and efficient patient flow protocols help maximize chair utilization while reducing waiting times. These improvements benefit both patient experience and practice productivity.
Administrative efficiency improvements can eliminate significant overhead costs that traditionally contribute to procedure pricing. Electronic health records, automated appointment scheduling, and streamlined billing processes reduce staff requirements and processing time. When these savings are substantial, they can support significant patient cost reductions.
Staff Productivity and Role Optimization
Maximizing staff productivity requires clear role definitions and systematic training that allows each team member to work at the top of their scope of practice. Dental assistants and hygienists can handle many routine aspects of endodontic care, allowing dentists to focus on procedures that require their specific expertise. This role optimization improves overall productivity and reduces per-procedure costs.
Cross-training programs help ensure consistent service delivery even when individual staff members are unavailable. When multiple team members can handle routine procedures and administrative tasks, scheduling becomes more flexible and patient care remains consistent. This operational reliability supports the volume-based approach that makes affordable care financially viable.
Performance measurement and feedback systems help maintain productivity standards while supporting staff development. Clear metrics for procedure time, patient satisfaction, and clinical outcomes provide objective feedback that supports continuous improvement. These systems become particularly important in high-volume practice environments where individual case attention might be limited.
Long-Term Sustainability and Market Impact
The long-term sustainability of affordable endodontic care models depends on achieving reliable patient volumes, maintaining clinical outcomes, and developing referral networks that support comprehensive dental care. These models represent a significant shift from traditional practice approaches, and their success requires careful attention to factors beyond immediate cost reduction.
Patient volume predictability becomes essential for maintaining reduced pricing structures. Affordable care models typically require higher patient volumes to offset reduced per-procedure revenue. Marketing, community outreach, and referral development become critical operational components that support the volume requirements necessary for sustainable pricing.
Clinical outcome tracking provides the evidence necessary to maintain credibility and support continued patient referrals. Successful affordable care programs invest in comprehensive outcome measurement and quality assurance systems that demonstrate treatment effectiveness. This data supports both patient confidence and professional referral relationships.
Community Health Impact
Accessible endodontic care can significantly impact community oral health by reducing the number of patients who delay or avoid necessary treatment due to cost concerns. When root canal therapy becomes financially accessible, fewer patients require emergency dental services or more expensive tooth replacement procedures. This preventive approach benefits both individual patients and the broader healthcare system.
Emergency department utilization for dental pain often decreases when affordable treatment options are available. Patients who can access timely, affordable endodontic care are less likely to seek emergency medical treatment for dental problems. This shift reduces healthcare system strain and provides more appropriate care for dental conditions.
Workforce productivity improvements result when employees can access affordable dental care without significant financial hardship. Dental pain and untreated endodontic problems can significantly impact work attendance and productivity. Accessible treatment options help maintain workforce health and reduce employer healthcare costs.
The evolution of affordable endodontic care represents a fundamental shift in dental service delivery that addresses long-standing accessibility barriers while maintaining clinical standards. Success requires systematic attention to operational efficiency, quality assurance, and sustainable practice management. As these models continue to develop, they offer the potential to significantly improve oral health access for working families while demonstrating that cost reduction and clinical quality can coexist in dental care delivery.